ahsmed
10 likes | 152 Views
Potential Primary Prevention Implantable Cardioverter -Defibrillator (ICD) Patients Lack Understanding, Want More Information and are Willing to Reconsider Implant Refusal. Narendra Singh MD , Erin Hall BSN , Essy Lucas BA, Sandeep Chandra MD, David H Song MD, Linda G Yan MD,

ahsmed
E N D
Presentation Transcript
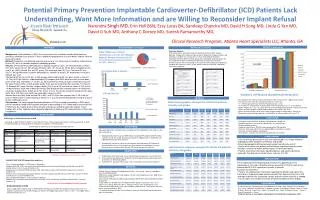
Potential Primary Prevention Implantable Cardioverter-Defibrillator (ICD) Patients Lack Understanding, Want More Information and are Willing to Reconsider Implant Refusal Narendra Singh MD, Erin Hall BSN, Essy Lucas BA, Sandeep Chandra MD, David H Song MD, Linda G Yan MD, David D Suh MD, Anthony C Dorsey MD, Suresh Ramamurthy MD, Clinical Research Program, Atlanta Heart Specialists LLC, Atlanta, GA ahsmed.com RESULTS (continued) BACKGROUND- continued ABSTRACT METHODS (continued) Statistical Analysis Statistical analyses were performed with the Microsoft Excel 2007 software package. Categorical variables are presented as frequencies and percentages and continuous variables are summarized as means and standard deviations. Differences between different ethnic groups were compared using Chi square test for categorical variables and ANOVA single factor for continuous variables Fischer exact test was used instead of chi square test when evaluating categorical variables with value less then 5. A two- sided p value of ≤ 0.05 was considered statistically significant. Ethnic Differences in Patient Characteristics, but not ICD Utilization Rates for Primary Prevention of SCD Presented AHA Resuscitation Symposium, Nov 2011 , Singh et al Background: Underutilization of ICD’s for primary prevention of sudden cardiac death has been previously reported in our practice. Factors leading to acceptance or refusal of device implant have not been well studied. Method: Prospective standardized interview and use of a 1-10 rating scale of randomly selected heart failure (HF) pts in a suburban outpatient cardiology practice. Results: Of the 533 HF pts identified with an ejection fraction of <35%, we interviewed 50. Of these 54% were Caucasian (C), 36% African American (AA), 10% Asian (A). 29 pts (58%) accepted an ICD and 21 pts (42%) refused, the “no ICD” group. The mean age was 62+11 yrs, The mean EF was 24+7%. No sig differences in patient demographics, cardiac risk factors, HF medications or baseline labwork was seen. Comparing ICD pts to no ICD pts- in both groups understanding of HF was poor, 4.5 on a scale of 1-10. The no ICD pts had less understanding of ICD purpose p<0.0003, were less likely to have been given written ICD information (71 vs 38%, p=.02) and were less likely to recall a recent discussion on the topic of ICD’s (52%). In both groups quality of life was more important than quantity, 7.7+3 out of 10. Although 93% were Christian, religious belief (3.3+3 out of 10) and cultural values (3.2+3 out of 10) did not play a major role in decision making. Both group felt they had great access to health care resources and physicians (8.5+2 out of 10). Only 2 (7%) of the ICD pts would not accept an ICD again, while 18 no ICD (86%) pts would now reconsider implant, p<0.001 Women were less likely to be married 26 vs 63%, p=0.02. A pts were younger than C, 56 vs 66 yrs, p=0.04. AA pts had less understanding of low EF vs C, p=0.02 and trended towards having less access to best medications p=0.1. Conclusions: Our study suggest that underutilization of ICD’s for primary prevention of SCD may in part be related to limited communication and poor understanding of HF sudden death and the devices. Furthermore the majority of pts initially refusing a device are willing to reconsider implant. These findings with further validation offer a potential approach to improving ICD underutilization in these high risk patients. P<0.001 ICD implant Men vs Women Summary of Physician Questionnaire Responses ICD and Ethnicity RESULTS - 85% of physicians felt they routinely talked to their pts re heart failure, sudden death, devices - These discussions were felt to be documented 72% of the time - 71% felt that giving literature on device implantation was useful - On a scale of 1-10 physicians ranked quality of life over quantity as 6.1 vs 7.7 by patients - Neither religion (2.8 + 2.6 ) or culture (4.0 + 2.8) influenced physician decision making extensively - Access to meds, hospitals and electrophysiologists was high 8.5 out of 10 - Access to insurance was felt to have a large negative effect on implantation 7.5 out of 10 -The patients cultural background had a neutral effect on offering a device 5.5 out of 10 Patient Demographics amongst ICD and No ICD patients, ethnicity, and gender BACKGROUND LIMITATIONS ICD Therapy in Primary Prevention of SCD - Descriptive study, Small but randomly selected patient sample size - Number of patients in certain ethnic groups was very small (Asians) - Single cardiology practice - Single inclusion criteria - EF≤35% was considered for ICD eligibility - Exclusion criteria eg. significant co-morbid conditions not always available - Interviews limited to English speaking pts - Survivor bias – only pts still alive were available to be interviewed According to MADIT, MUSTT, MADIT II and SCD HeFT Trials ICD therapy found effective in primary prevention of SCD in treatment groups by showing significant reduction in mortality in treatment groups Clinical features and results of four primary prevention ICD trials HYPOTHESIS Many potential factors contribute to the acceptance of ICD implantation. Our study is a two part evaluation to: Retrospectively look through our EMR charts of potential HF patients with EF≤ 35% to study the rate of ICD usage for primary prevention in eligible patients stratified by self reported ethnicity. (previous abstract) Prospectively, interview a subset of these patients with and without ICD implant to understand the reasons for their decisions. Also question the cardiologists to see if physician factors influence them offering ICD device therapy (this abstract) CONCLUSIONS • ICDs for primary prevention of SCD are underutilized in this single suburban cardiology practice regardless of ethnicity and gender • Patient demographics differed amongst gender and ethnicity, p<0.01 • Quality of life rather than quantity mattered more to patients than physicians • Religious and cultural beliefs did not impact ICD decisions greatly • Patients want more information regarding devices and would significantly reconsider their decision to initially refuse a device. P<0.001 Questionnaire responses amongst ICD and No ICD patients, ethnicity, and gender OBJECTIVES Table adopted from-- Welsenes G H van. Neth Heart J 2011 Jan; 19(1)24-30. • To determine what factors play a role in determining acceptance or refusal of an ICD • 2. To characterize and determine if disparity in ICD therapy for primary prevention exists on the basis of ethnicity or gender • 3. To determine if physician factors play a role in offering an ICD to potential patients IMPLICATIONS AHA/ACC/HRS 2008 ICD Implantation guidelines These finding add to the growing body of literature suggesting that ICD implantation is still under utilized for primary prevention of SCD in heart failure patients with EF≤ 35% regardless of gender or ethnicity Based on our interviews; • Patients are seeking more information regarding the devices and if given this information a large percentage would reconsider their decision to refuse an ICD • Attempts to deliver this information verbally and with written materials is needed • Future studies are needed to evaluate the generalizability of these findings Class I Recommendations - ICD therapy is indicated in ; Patients with LVEF ≤ 35% due to prior myocardial infarction who are at least 40 days post MI and are in NYHA functional Class II or III. (Level of Evidence: A) Patients with non ischemic DCM who have LVEF ≤35% and who are in NYHA functional class II or III. (Level of Evidence: B) Patients with LV Dysfunction due to prior MI who are at least 40 days post MI and have LVEF<30% and are in NYHA functional class I.(Level of Evidence: A) Class IIb Recommendations - ICD may be considered in Patients with no ischemic heart disease who have LVEF ≤ 35% and who are in NYHA functional Class I. (Level of Evidence : C) METHODS • Setting - Single suburban Cardiology practice with 4 sites having 7 general cardiologists but no electrophysiologist. • EMR charts review of patients with diagnosis of heart failure beginning in Jan. 2006 to Dec 2010 5 years N=2813 • Out of those 2813 patients, EMR charts of patients with EF≤35% were abstracted in detail N=533(19%) • Study cohort was divided into 5 self reported ethnic groups: Caucasians (23%), East Indians (3%), African Americans (67%), South East Asian s(6%) and Hispanics (2%) • From this cohort 50 patients (10%) were randomly selected for an 1 hour phone interview with a single trained nurse (EH) • A standardized questionnaire using a 10 point scale was utilized and free text comments were also recorded DISCLOSURES Epstein AE et al, Circulation2008 May 27;117(21); e350-408 Underutilization of ICDs DrNarendra Singh- Research grants from Medtronic, St Judes, Sorin, Biotronik, Erin Hall-None, Essy Lucas- now works for Medtronics in diabetes division, Dr Sandeep Chandra – None, Dr David H Song – None, Dr Linda G Yan – None, Dr David D Suh – None, Dr Anthony Dorsey – None, Dr Suresh Ramamurthy – None Funded in part by an investigator-initiated grant from MedtronicsCorporation, USA Between 2005-2007, analysis done on AHA’s GWTG-HF Registry (Get With The Guideline-Heart Failure) from 217 hospitals found that the use of ICD therapy was lower in the eligible black patients (23.0% vs 69.1% for eligible whites) and in the women (27.2%)