INTRODUCTION
Impact of Film Properties and Drug Physicochemical Properties on Diffusion through a Poly (Vinyl Alcohol) Film for the Development of GIRES TM.

INTRODUCTION
E N D
Presentation Transcript
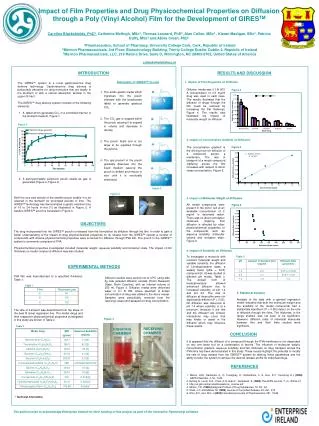
Impact of Film Properties and Drug Physicochemical Properties on Diffusion through a Poly (Vinyl Alcohol) Film for the Development of GIRESTM Caroline Blackshields, PhD1, Catherine McHugh, MSc2, Thomas Leonard, PhD3, Alan Cullen, MSc2 , Kieran Madigan, BSc2, Patricia Duffy, MSc2 and Abina Crean, PhD1 1Pharmaceutics, School of Pharmacy, University College Cork, Cork, Republic of Ireland 2Merrion Pharmaceuticals, 3rd Floor, Biotechnology Building, Trinity College Dublin, Dublin 2, Republic of Ireland 3Merrion Pharmaceuticals, LLC, 219 Racine Drive, Suite D, Wilmington, NC 28403-8702, United States of America c.blackshields@ucc.ie RESULTS AND DISCUSSION INTRODUCTION 1. Impact of Film Properties on Diffusion Schematic of GIRESTMin-vivo • The GIRES™ system is a novel gastroretentive drug delivery technology. Gastroretentive drug delivery is particularly attractive for drug molecules that act locally in the stomach or with a narrow absorption window in the upper GI tract. • The GIRES™ drug delivery system consists of the following elements: • A tablet which generates CO2 in a controlled manner in the stomach medium, Figure 1. • A semi-permeable polymeric pouch swells as gas is generated (Figure 2, Figure 3). Figure 4 Diffusion media was 0.1 N HCl. A concentration of 0.5 mg/ml drug was used in each case. The results illustrated that the diffusion of drugs through the film could be reduced by increasing the film thickness, Figure 4. The results also illustrated the impact of molecular weight on diffusion. • The acidic gastric media which ingresses into the pouch interacts with the bicarbonate tablet to generate gaseous CO2. • The CO2 gas is trapped within the pouch causing it to expand in volume and decrease in density. • The pouch floats and is too large to be expelled through the pylorus. • The gas present in the pouch gradually dissolves into the liquid medium causing the pouch to deflate and reduce in size until it is eventually eliminated. Figure 1 2. Impact of Concentration Gradient on Diffusion The concentration gradient is the driving force for diffusion of a compound across a membrane. The rate of transport of a model compound (caffeine) across the film increases with respect to donor vessel concentration, Figure 5. Figure 5 Figure 2 Figure 3 Both the size and density of the swollen pouch enable it to be retained in the stomach for prolonged periods of time. The GIRESTM technology has demonstrated a gastric retention time of 16 to 24 hours in-vivo [1] as illustrated in Figure 2. A swollen GIRESTM pouch is illustrated in Figure 3. 3. Impact of Molecular Weight on Diffusion All model compounds were present in the donor cell at an available concentration of 2 mg/ml in deionised water. There was no direct correlation observed, implying that diffusion is affected by other physicochemical properties of the compounds, such as aqueous solubility, molecular volume and ionisation state, Figure 6. Figure 6 OBJECTIVES The drug incorporated into the GIRES™ pouch is released from the formulation by diffusion through the film. In order to gain a better understanding of the impact of drug physicochemical properties on its release from the GIRESTM system a number of compounds with diverse physicochemical properties were screened for diffusion through PVA film. The pouch in the GIRES™ system is commonly composed of PVA. Physicochemical properties investigated included molecular weight, aqueous solubility and ionisation state. The impact of film thickness on model compound diffusion was also studied. 4. Impact of Solubility on Diffusion To investigate a molecule with constant molecular weight and variable solubility, the diffusion of Levobupivacaine base, a weakly basic (pKa = 8.03) compound [4, 5] was studied in different pH media, Table 3. The ionised form of levobupivacaine showed enhanced diffusion due to increased solubility at pH 1.2 and pH 4.0. The rate of diffusion at these pHs were not significantly different (P > 0.05). No diffusion was observed at pH 7.4 where solubility is at a minimum. However if the film and the diffusant are ionised, interactions may occur that may hinder or assist in the diffusion which may influence these results . Table 3 EXPERIMENTAL METHODS PVA film was manufactured to a specified thickness, Table 1. Diffusion studies were carried out at 37oC using side by side jacketed diffusion vessels (Prism Research Glass, North Carolina), with an internal volume of 250 ml, Figure 3. Diffusion media were deionised water or 0.1 N HCl, where specified. A known concentration of drug was added to the donor vessel. Samples were periodically removed from the receiving vessel and assayed for drug concentration. Table 1 5. Statistical Analysis Analysis of the data with a general regression model indicated that both the molecular weight and the solubility of the model compounds had a statistically significant (P < 0.05) impact on the rate of diffusion through the films. The thickness, in the range studied, was not seen to be significant. However, diffusion rates of individual molecules between thin and thick films studied were significant. The rate of transport was determined from the slope of the best fit linear regression line. The model drugs and their respective physicochemical properties investigated in this study are shown in Table 2. Figure 3 Table 2 RECEIVING CHAMBER DONATING CHAMBER CONCLUSION It is apparent that the diffusion of a compound through the PVA membrane is not dependant on any one factor but on a combination of factors. The influence of molecular weight, concentration gradient, aqueous solubility and film thickness on drug transport across the PVA films has been demonstrated in this study. These results highlight the potential to modify the rate of drug release from the GIRESTM system by altering these parameters and the ability to tailor the system to achieve the desired release profile for individual drugs. REFERENCES 1.Wilson, A.M., Ramtoola, Z., O. Conaghey, O., McGoldrick, C. A., Hou, S.Y., Cumming, K.I. (2002) AAPS PharmSci, 4, S1, 1045 2. Rytting, E, Lentz, K.A., Chen, X-Q, Qian F., Venkatesh, S. (2005) The AAPS Journal,7, (1), Article 10 3. http://us.gsk.com/products/assets/us_zovirax.pdf 4. Wilson, T.D. (1990) Analytical Profiles of Drug Substances, 19, 59 - 94 5. Shah, J.C. and Maniar, M. (1993) Journal of Controlled Release, 23, 261- 270 6. Shin, S-C. and Kim, J.(2003) International Journal of Pharmaceutics, 251, 79-84 * Technical Information. The authors wish to acknowledge Enterprise Ireland for their funding of this project as part of the Innovative Partnership Initiative