Neovascular Glaucoma (NVG)
Neovascular Glaucoma (NVG) Saleh A. Al-Obeidan, MD Department of Ophthalmology College of Medicine King Saud University Neovascular Glaucoma (NVG) Neovascular Glaucoma is one of the most

Neovascular Glaucoma (NVG)
E N D
Presentation Transcript
Neovascular Glaucoma(NVG) Saleh A. Al-Obeidan, MD Department of Ophthalmology College of Medicine King Saud University
Neovascular Glaucoma(NVG) • Neovascular Glaucoma is one of the most • Challenging forms of secondary glaucomas. It occurs when the fibrovascular tissue proliferates onto the chamber angle, obstructs the trabecular meshwork, and produces peripheral anterior synechiae and progressive angle closure. The elevated intraocular pressure is often difficult to control and frequently results in loss of vision.
NVG Pathogenesis Leading causes: • Retinal Ischemia Responsible for 97% - Diabetic Retinopathy - Central Retinal Vein Occlusion Brown GC et al. Ophthalmology 1984
NVGPathogenesis • X-Factor • VEGF - Vascular Endothelial Growth Factor 1 of 9 non polypeptide growth factors Specific for endothelial cells (EC) Causes EC migration and mitosis Increases EC permeability
NVGPathogenesis • VEGF (source in the eye) Expressed and produced by: Corneal endothelium, Iris pigment epithelium, RPE, Ganglion cells, Astrocytes, Muller cells, Uveal melanocyte, and Choroidal fibroblasts. J Glaucoma 2002
NVGPathogenesis • VEGF Markedly elevated in aqueous humor of patients with NVG. Diabetes Care Nov. 1996 Ophthalmology 1998 J Glaucoma 2002
NVGPathogenesis • VEGF(210 Vitrectomy samples) - Vitreous (VEGF) PDR 36x NPDR - Vitreous (VEGF) > Aqueous (VEGF) - (VEGF) 75% post PRP • VEGF plays a major part in mediating active intraocular neovascularization in patients with ischemic retinal diseases. N Engl J Med 1994;331:1480-7
NVGPathogenesis Anti Angiogenic Therapy: Intravitreal injection of crystalline cortisone causes regression of iris neovascularization Jonas et al. J Glaucoma 2001
NVGPathogenesis Anti-Angiogenic Therapy: Anti VEGF (Ranibizumab, Lucentis) Intravitreal injection prevented formation of CNV in monkeys and decreased leakage of already formed CNV with no significant toxic effects Arch Ophthalmol 2002 Kim, et al. Invest Ophthalmol. Vis Sci 2006
NVGPathogenesis Anti Angiogenic Therapy: Anti VEGF [SU 5416 (Semaxinib)] Durable and rapid recovery of visual functions in a patient with von Hippel-Lindau syndrome Ophthalmology, Feb 2002 J Clin Oncol. May 2005
NVGPathogenesis Anti Angiogenic Therapy: Anti VEGF [Aptamer (Macugen)] Remarkable reduction in the size of CNV Remarkable visual improvement “26.7% gained 3 lines or more” The Eye Tech Study Group, Retina 2002 Exp Eye Res. May 2006 Ophthalmology. Apr 2006
NVGPathogenesis Anti Angiogenic Therapy: Bevacizumab [Avastatin] Davidorf, et al. Retina 2006 Kehook, et al. Ophtha Surg 2006
NVGPathogenesis Panretinal Photocoagulation and Ocular Neovascularization PRP upregulate expression of transforming growth factor- (TGF- ) TGF- is a powerful vascular endothelial cell proliferation inhibitor. Invest Ophthalmol Vis Sci 1998
NVGPathogenesis Panretinal Photocoagulation and Ocular Neovascularization Photo coagulated cultured human RPE & rat retinas upregulate expression of high level of Pigment Epithelium Derived Factor (PEDF) PEDF has been shown to be a potent inhibitor of ocular angiogenesis Am J Ophthalmol, Sep 2001 Am J Ophthalmol Aug 2002 Invest Ophthalmol Vis Sci 2002
NVGPathogenesis Panretinal Photocoagulation and Ocular Neovascularization Major benefit of PRP may be destruction of VEGF source.
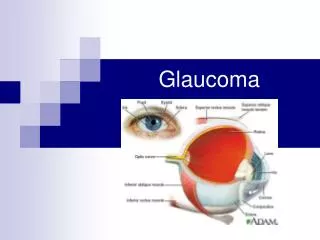
NVG Clinical Presentation • Reduced vision • Injected eye • A/C reaction • Elevated IOP < 40 mmHg • Middilated, non reactive pupil • Rubeosis irides (NVI) • Neovascularization of the angle (NVA)
NVG • Enucleation is only practical treatment • No means are known to prevent NVG • The treatment of NVG is disheartening Duke Elder, 1969 Grant, 1974 Hoskins, 1974
NVG • Outcomes have improved dramatically. • New medical and surgical approaches. • Better understanding and control of angiogenesis.
NVG “If the neovascular element can be removed and further neovascularisation prevented, then we are left with an uncomplicated angle-closure problem which should be amenable to classical drainage surgery.” Flanagan D.W. & Blach R.K. Br J. Ophtamol 1983;67,526-8
NVG Management • Recognition of patients at HIGH RISK • Recognition of NVI before angle closure is critical • Treatment
NVG Management • Recognition high risk patients • Correction of the underlying pathology • Close observation (NVI & NVA) • Efficient & sufficient PRP • Prevention: • Treatment
NVG Treatment • Visual potential • Clarity of the media Determinants
NVG Treatment (cont.) • Control inflammation & pain • Cycloplegia • Steroids Medical Therapy
NVG Treatment (cont.) • Control IOP • Aqueous suppressants • Avoid miotics & prostaglandines Medical Therapy
NVG Treatment (cont.) • Panretinal photocoagulation (PRP) • 1st line of therapy (if possible) • Reduces & can eliminate ant. seg. neovascularization. • Panretinal cryoablation Laser Therapy Cryo Therapy
NVG Treatment (cont.) • Filteration surgery • Tube surgery • Cyclodystructive procedures • Others Conventional Surgery
NVGTreatment Cyclodestructive procedures: High rate of serious complications and visual loss • Cyclophotocoagulation Visual loss up to 46.6% Shields & Shields 1994 • Cyclocryotherapy Visual loss of up to 70% Caprioli et al. Ophthalmology 1985 • Phthisis Bulbi 34% Krupin T et al. Am J Ophthalmol 1978;86:24-6
NVGTreatment Tube shunts: • Variable success rates • Probably more suitable for previously operated eyes (e.g. failed filter proced. Aphakia) • High rate of visual loss (19-48%) and phthisis bulbi (11-25%) Mermoud et al. Ophthalmology 1993
NVG Treatment (cont.) • Filteration surgery
Full PRP Improves the Outcome of Trabeculectomy in NVG Surgical Technique Procedure - Standard Trabeculectomy - Mitomycin “C” 0.2mg/ml/2mins. Precautions - Gradual decompression of the eye
Full PRP Improves the Outcome of Trabeculectomy in NVG • Short Term Complications: • - Transient hypotony - 14/23 (61%) • - Hyphema - 8/23 (35%) • - Choroidal Detachment - 2/23 (9%) • - Leaking Bleb - 1/23 (4%) • Long Term Complications: • - Cataract prog. – 2/23 (9%) • - NLP • - Hypotony Maculopathy Non • - Phthisis Bulbi
Full PRP Improves the Outcome of Trabeculectomy in NVG Results Complete Success 20/23 (87%) Qualified Success 3/23 (13%)
Treatment NVG NLP - Medical Rx - Cyclodestructive procedure Seeing eye Vitreous hge Vitrectomy+ endolaser Clear media PRP Poor media Cryoablation Trabeculectomy & Mitomycin Not suitable for trab. Tube shunts cyclophotocoagulation
NVGPoints to Remember It is a preventable condition.
NVGPoints to Remember It is a treatable condition.