IVF
IVF. Dr. H. R. Muharam, SPOG (K). Introduction. In vitro fertilization ( IVF ) is a process by which egg cells are fertilised by sperm outside of the womb, in vitro . IVF is one method of assisted reproductive technology. No cause. More than one. Male factor. Endometriosis.

IVF
E N D
Presentation Transcript
IVF Dr. H. R. Muharam, SPOG (K)
Introduction • In vitro fertilization (IVF) is a process by which egg cells are fertilised by sperm outside of the womb, in vitro. • IVF is one method of assisted reproductive technology
No cause More than one Male factor Endometriosis Dysovulation Unexplained Tubal factor Figure 1 The causes of infertility in a large observational multicenter study in the UK, 2003 McVeigh,ASRM, 2004
* In these situations intrauterine insemination treatment merits consideration before proceeding to IVF
Introduction • The first IVF baby in the world (Louise Brown) was born in July of 1978 in England. • Louise Brown was 28 when she delivered her own baby in 2006. Her baby was conceived without IVF. Hundreds of thousands of children are now born annually as a result of the IVF technique
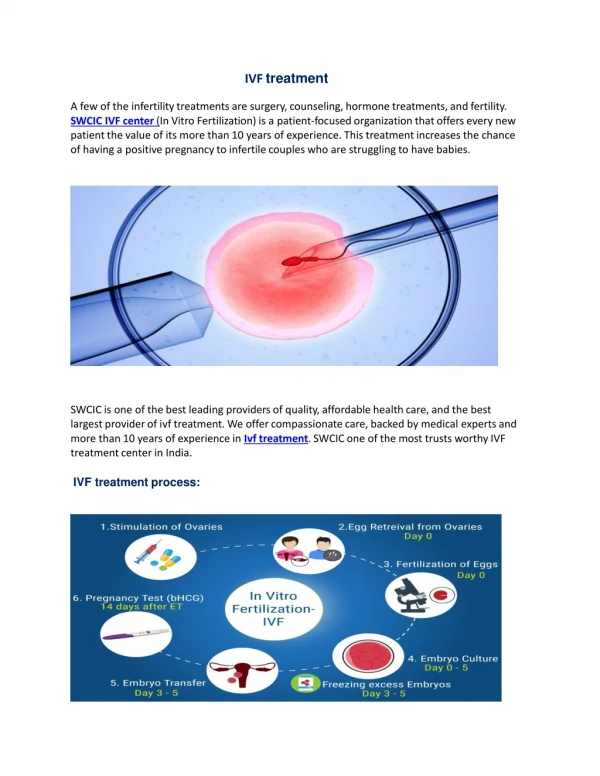
The process involves : • Hormonally controlling the ovulatory process • Removing ova (eggs) from the woman's ovaries • Letting sperm fertilise them in a fluid medium. • The fertilised egg (zygote) is then transferred to the patient's uterus with the intent to establish a successful pregnancy
Problems of the fallopian tube, but it turned out that it was successful in many other infertility situations as well. • The introduction of intracytoplasmic sperm injection (ICSI) addresses the problem of male infertility to a large extent. • This means that IVF can be used for females who have already gone through menopause.
Indication • An anatomic problem with the uterus, such as severe intrauterine adhesions • Blocked fallopian tubes or pelvic adhesions • tubal reversal surgery • vasectomy reversal surgery • Male factor infertility (low sperm count or low motility). • ICSI is an IVF procedure that can fertilize eggs even with poor sperm quality. • Failed 2-4 cycles of ovarian stimulation with intrauterine insemination • Advanced female age - over about 38 years of age. • Severe endometriosis • Unexplained infertility when inseminations have failed - unexplained infertility means standard fertility tests have not found the cause of the fertility issue
Method Ovarian stimulation • Started on the third day of menstruation and consist of a regimen of fertility medications to stimulate the development of multiple follicles of the ovaries • Monitoring • Estradiol • USG, follicular growth. Typically approximately 10 days of injections will be necessary. • Spontanenous ovulation during the cycle is prevented by the use of GnRH agonists or GnRH antagonists, which block the natural surge of luteinising hormone (LH).
Stimulation protocol Three types of drugs: • GnRH-agonist (gonadotropin releasing hormone agonist) or a GnRH-antagonist (e.g. Ganirelix) to suppress the LH surge and ovulation until the follicles are mature • FSH product (follicle stimulating hormone) to stimulate development of multiple follicles • HCG (human chorionic gonadotropin) to cause final maturation of the eggs in the follicles • The purpose of the GnRH-agonist (or antagonist) is to suppress release of LH (luteinizing hormone) from the woman's pituitary gland during the ovarian stimulation process. LH surges would cause premature ovulation (release) of the eggs. • The purpose of the FSH product is to stimulate development of multiple follicles (structures that contain eggs) in the ovaries.
Ovarian Stimulation Protocols Using GnRH-agonists • "Long protocols", also called "luteal Lupron", or "down regulation" protocols • "Flare" protocols, also sometimes called "short" protocols
Long Protocol IVF Hari pertama haid lapor Buserelin nasal 3 kali setiap hari Transfer embrio Ovum Pick up hCG malam Suntikan gonadotropin Tes urin Tiap hari 1 3 21 36 jam ± 2 mg 2 hari 14 hari ± 2 mg Pemeriksaan USG vag Hormonal Usg vag darah Suami siap
Egg retrieval • When follicular maturation is judged to be adequate, • human chorionic gonadotropin (β-hCG) is given. • Acts as an analogue of luteinising hormone • The eggs are retrieved from the patient using a transvaginal technique involving an ultrasound-guided needle piercing the vaginal wall to reach the ovaries. • The retrieval procedure takes about 20 minutes and is usually done under conscious sedation or general anesthesia
Ovum Pick Up • Aspirasi folikel • Pencarian sel telur
Fertilisation • Eggs are stripped of surrounding cells and prepared for fertilisation., • Semenis prepared for fertilisation by removing inactive cells and seminal fluid. • The sperm and the egg are incubated together (at a ratio of about 75,000:1) in the culture media for about 18 hours. • By that time fertilisation should have taken place • The fertilised egg would show two pronuclei. • In situations where the sperm count is low, a single sperm is injected directly into the egg using intracytoplasmic sperm injection (ICSI). • The fertilised egg is passed to a special growth medium and left for about 48 hours until the egg has reached the 6-8 cell stage.
ICSI Intracytoplasmic Sperm Injection diperlukan hanya 1 sperma motil saja untuk disuntikkan kedalam ooplasma
Simpan Beku • Sperma • Embrio
Selection • Laboratories have developed grading methods to judge oocyte and embryo quality • Typically, embryos that have reached the 6-8 cell stage are transferred three days after retrieval or embryos are placed into an extended culture system with a transfer done at the blastocyst stage, especially if many good-quality day-3 embryos are available. • Blastocyst stage transfers have been shown to result in higher pregnancy rates.[1]. In Europe, transfers after 2 days are common.
Sperma Suami • Persiapan sperma suami
Embryo Transfer • Embryos are graded by the embryologist based on the number of cells, evenness of growth and degree of fragmentation. • The number to be transferred depends on the number available. • In the UK and according to HFEA regulations • > 40 may have up to three embryos transferred, • Younger women may have many embryos transferred based on individual fertility diagnosis. • Most clinics and country regulatory bodies seek to minimise the risk of pregnancies carrying multiples. • The embryos judged to be the "best" are transferred to the patient's uterus through a thin, plastic catheter, which goes through her vagina and cervix.
Transfer embrio • Penentuan hari transfer • Persiapan transfer embrio
Complications • The major complication of IVF is the risk of multiple births.[2] • Increased risk of pregnancy loss, • obstetrical complications, prematurity, and • neonatal morbidity with the potential for long term damage • Spontaneous splitting of embryos in the womb after transfer can occur, but • Ovarian stimulation is the development of ovarian hyperstimulation syndrome.
Monitoring Pasca Transfer Embrio • Luteal suppport • USG • Monitoring sampai 12 minggu
Komplikasi • Ovarium hiperstimulasi • Kehamilan ektopik • Perdarahan
Table 32.3. Impact of cause of infertility on livebirth rate from IVF. Templeton AA, et.al, Lancet 1996
Correlation between female age and pregnancy rate 1427 IVF cycles in UK in 2003