MUSCLE TISSUE
MUSCLE TISSUE. MUSCLE TISSUE. A primary tissue type, divided into: skeletal muscle cardiac muscle smooth muscle. Connective Tissue Organization . 1. Epimysium Exterior collagen layer Surrounds entire muscle Separates muscle from surrounding tissues 2. Perimysium

MUSCLE TISSUE
E N D
Presentation Transcript
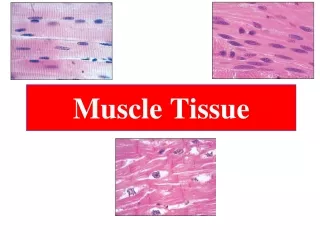
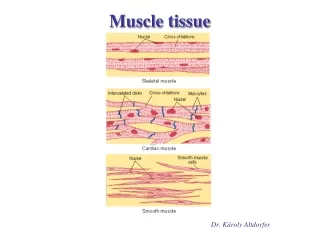
MUSCLE TISSUE • A primary tissue type, divided into: • skeletal muscle • cardiac muscle • smooth muscle
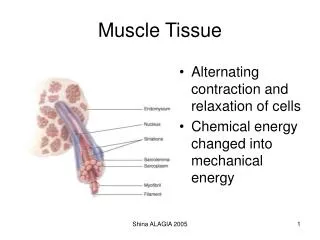
Connective Tissue Organization 1. Epimysium • Exterior collagen layer • Surrounds entire muscle • Separates muscle from surrounding tissues 2. Perimysium • Surrounds muscle fiber bundles (fascicles) • Contains blood vessel and nerve supply to fascicles
3. Endomysium • Surrounds individual muscle cells (muscle fibers) • Contains capillaries and nerve fibers contacting muscle cells • Contains satellite cells (stem cells) that repair damage • Endomysium, perimysium, and epimysium come together at ends of muscles to form connective tissue attachment to bone matrix i.e., tendon.
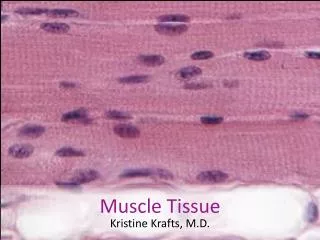
SKELETAL MUSCLE CELL • Striated/striped appearance of skeletal muscle cell is due to the orderly arrangement of the thin and thick filaments . that makeup the majority of the contractile proteins. • The contractile proteins are made of 3 types of filaments; 1. THIN FILAMENT 2. THICK FILAMENT 3. ELASTIC FILAMENT
CONTRACTILE PROTEINS • THIN FILAMENT • Thin filament is placed hexagonally around myosin • Make and break contacts with myosin during contraction • Has 3 parts; i) ACTIN PROTEIN (i.e. the main molecule of this filament). FUNCTION: Binds to myosin head.
CONTRACTILE PROTEINS ii) TROPONIN FUNCTION: Regulatory function by binding to Ca 2+ iii) TROPOMYOSIN FUNCTION: Has a regulatory function by blocking/unblocking the binding site of actin to the myosin head
CONTRACTILE PROTEINS • THICK FILAMENT • Thick filament: composed of structural protein, myosin. - has 2 main parts • Myosin head - possesses actin binding site and ATPase activity. ii) Myosin tail– forms the shaft of thick bands.
CONTRACTILE PROTEINS 3. ELASTIC FILAMENT – made of titin molecule FUNCTION: – Fixes the thick filament to a z disc.
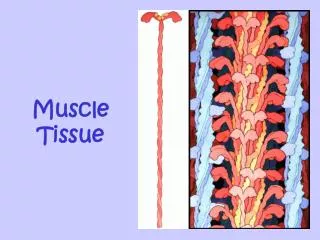
Muscle Sarcomere • Sarcomere - functional unit of muscle cell • Consist of thick and thin filaments – myofilaments/ myofibril • Myofilaments that lies between two ‘z’ lines- sarcomere • - Dark & light bands alternate • - Light I band is Isotropic • - Dark A band is anisotropic • - Z line bisects I band • - H zone: No overlap of actin
Myofibrils • Each myofibril consists of two types of protein filaments -"thick filaments", and "thin filaments". • Thick filaments and the thin filaments within myofibrils overlap in a structured way, forming units called sarcomeres. • Sarcomeres are sections of myofibril that are separated from each other by areas of dense material called "Z discs".The sarcomeres are also described in terms of the bands/zones within which one or both of the two filaments occur.
The "A band" is a relatively darker area within the sarcomere that extends along the total length of the thick filaments. • The "H zone" is at the centre of the A band of each sarcomere. As shown below, this is the region in which there are only thick filaments, and no thin filaments.The "I band" is the region between adjacent A bands, in which there are only thin filaments, and no thick filaments. ( Each I band extends across two adjacent sarcomeres.)
Muscle contraction [SLIDING FILAMENT THEORY] • Involves the sliding of the actin over the myosin which causes the muscle to shorten and therefore develop tension • The process of muscular contraction can be explained by the sliding filament theory
Muscle contraction [SLIDING FILAMENT THEORY] Excitation: Step 1 • Action potential (AP) travels to nerve ending • ACh release at the neuromuscular junction • Activation of receptors by ACh • Voltage gated Na channels open • AP is generated in the muscle fiber
Muscle contraction • Depolarization of sarcolemma • Action potential transmitted down T-tubule • Sarcoplasmic reticulum releases Ca++ • Ca++ binds to troponin C • Active actin site is exposed
Muscle contraction Contraction: Step 2 • Myosin heads are activated Myosin head hydrolyses (breakdown) ATP to release energy Myosin head gains energy so it becomes activated. Activated myosin head is ready to bind with actin filament (cross bridge)
Muscle contraction 2. Activated myosin head binds rapidly to myosin- binding sites on actin 3. Myosin head still bonded to actin; i) Changes its shape ii) Moves towards the center of sarcomere Above steps, i) and ii) called power stroke 4. Myosin head is still bonded to actin
Muscle contraction 5.ATP binds to the myosin in the myosin-actin complex 6. Myosin head detaches from actin 7. Myosin head hydrolyses ATP to release energy. 8. Steps 2 – steps 8 is repeated • During muscle contraction the thin actin filaments slide over the thick myosin filament. • This results in a reduction in the distance from Z line to Z line • H zone increases while while I band decreases.
Muscle contraction Relaxation: Step III • Ca++ is pumped back to sarcoplasmic reticulum • Active pump utilizing ATP • Actin sites are covered by troponin • Ca++ remains stored in the reticulum
NEUROMUSCULAR JUNCTION • Each muscle fibre is connected to a nerve fibre branch coming from a nerve cell. • These nerve cells are called motor neurons, and extend outward from the spinal cord • The motor neuron and all the muscle fibres it innervates are called a motor unit. • Stimulation from motor neurons initiates the contraction process. • The site at which motor neuron attaches on the muscle cell is known as the neuromuscular junction
NEUROMUSCULAR JUNCTION • At this junction, the sarcolemma forms a pocket known as the motor end plate • The end of the motor neuron is not in direct contact with the muscle fibre but is separated by a short gap known as the neuromuscular cleft • A nerve impulse reaching the end of the motor nerve stimulates the release of the neurotransmitter acetylcholine which diffuses across the synaptic cleft and binds to the receptor sites on the motor end plate
NEUROMUSCULAR JUNCTION • This causes an increase in permeability of sarcolemma to sodium and sodium diffuses into muscle fibre resulting in a depolarisation called the end-plate potential (EPP) • This EPP is usually large enough to exceed the threshold that is the signal to start the contractile process.