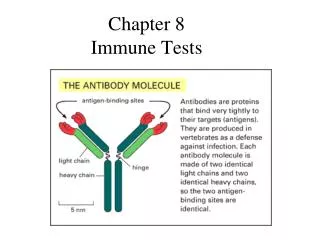
Chapter 8 Immune Tests
Chapter 8 Immune Tests. Immuno diagnostic Studies. Studies antigen-antibody reactions for diagnosis of infectious disease, autoimmune disorders and immune allergies. Also Blood groups and types , tissue graft transplant matching and cellular immunology. Antibodies.

Chapter 8 Immune Tests
E N D
Presentation Transcript
Immuno diagnostic Studies Studies antigen-antibody reactions for diagnosis of infectious disease, autoimmune disorders and immune allergies. Also Blood groups and types , tissue graft transplant matching and cellular immunology.
Antibodies Are proteins produced by the bodies immune system in response to an antigen or antigens. The antigen-antibody response is bodies natural response to invading organisms
Antigen Are substances that stimulate and subsequently react with the products of immune response. They may be enzymes, toxins, microorganisms (bacteria,fungus,virus etc.) tumors or autoimmune factors
Autoimmune disorders Autoantibodies, that is antibodies against self
Immunodeficiency diseases Exhibit a lack of one or more components of the immune system, which includes B, T lymphocytes, phagocytic cells, and the complement system. Primary(congenital DiGeorg’s syndrome) and Secondary(AIDS)
Immune deficiencies Burton’s agammaglobulinemia B cell deficiency (asociated with recurrent bacterial infections after 6 months)
Thymic aplasia (Di george’s syndorme) T cell deficiency (recurrent parasitic,viral and protozoal infections)Chronic Muco-cutaneous candidiasis T cell dysfunction specifically for candida albicans.
Autoantibodies • ANA • Anti-Centromere antibody • Rheumatoid factor • Carcino-Embryonic antigen • APAS • Anti-microsomal antibody/TPO antibody • Anti-mitochondrial antibodies • Anti-parietal cell antibodies • Glomerular basement membrane antibodies • Anti-Gliadin antibodies • ANCA, anti insulin antibodies • Anti-Post synaptic acetylcholine receptor antibodies
ANA Autoantibodies are directed towards nuclear material (ANA’s) or to cytoplasm. Many abnormal antibodies are present with autoimmune (rheumatic) disease. ANA is a group of protein antibodies that react against cellular nuclear material, it is sensitive for detecting SLE (95%) , but also detected in other rheumatic disorders , therefore it is not specific.
ANA Homogenous pattern Diffuse SLE (-non specific) Outline pattern SLE Speckled pattern non-specific Nuclear pattern Scleroderma, polymyositis
Why the test is performed ? This test is used when autoimmune disease is suspected (particularly systemic lupus erythematosus). This test can also be performed when a patient has unexplained symptoms such as arthritis, rashes, or chest pain.
The presence of ANA in the blood may indicate: • SLE (systemic lupus erythematosus) • Drug-induced lupus erythematosus • Collagen vascular disease • Myositis (inflammatory muscle disease) • Chronic liver disease • Rheumatoid arthritis • ANA may also be present occasionally in people with: Systemic sclerosis (scleroderma)Thyroid disease
The presence of ANA in the blood may also indicate: • The ANA can be positive in relatives of those with SLE who do not have SLE themselves. • Also, many drugs affect the accuracy of this test. Examples are: birth control pills, Procainamide, and thiazide diuretics.
Anticentromere Antibody Appear is 90% of CREST syndrome (variant of scleroderma) Scleroderma: Excessive fibrosis and collagen deposition throughout the body, affecting skin , cardiovascular , kidney and GI systems 1-Diffuse scleroderma (skin and viscera) 2-C(calcinosis) R(Raynauds phenomenon) E(esophageal dysmotility) S (sclerodactyly) T(telangiectasia)
Rheumatoid Arthritis common in females, 80% have positive Rheumatoid Factor (anti-IgG Ab) Classic presentation : morning stiffness improving with use , symmetric joint involvement and systemic symptoms : fever, fatigue, pleuritis, pericarditis.
Rheumatoid Arthritis 1-Morning stiffness 2-Arthritis in 3 or + joints (PIP-MCP-wrist-elbow-knee-ankle-MTP 3-Arthritis in hand 4-Symmetrical arthritis 5-Rheumatoid nodules 6-Serum rheumatoid factor 7-Radiographic changes 4 of seven criteria . 1-4 for 6 weeks
RADIOLOGY Rheumatoid Arthritis Loss of bone in periarticular areas Erosion (loss of bone in margins) Joint space narrowing (due to cartilage loss)
DefinitionRheumatoid factor is a test that measures the presence and level of rheumatoid factor (RF) in the blood. The RF test is used mainly in the diagnosis of rheumatoid arthritis, although the test result can be positive in many other diseases as well as in healthy people. RF is an antibody that attaches to immunoglobulin G (IgG), forming a molecule known as an immune complex. This immune complex can activate various inflammatory processes in the body. About 80% of patients with rheumatoid arthritis have positive RF tests.
Carcinoembryonic Antigen Carcinoembryonic antigen (CEA) is a family of glycoproteins encoded on chromosome 19. It was first observed in extracts of colonic carcinoma tissue. Elevated levels are found in serum from patients with a wide variety of tumor types including GI, lung, breast, ovary, and uterus.
High levels are more likely in the presence of metastatic disease and prognostically indicate a greater likelihood of metastasis.
CEA is most useful in monitoring patients for tumor recurrence and therapeutic efficacy. Levels will usually fall following successful treatment and remain stable. Rising levels in these patients may indicate recurrence.
CEA is often elevated in liver disease, and smokers may have slightly elevated levels of CEA.
(APS) Antiphospholipid antibodies
(APS) The antiphospholipid antibody syndrome (APAS) is currently recognized as a common risk factor for arterial or venous thromboembolic disease. These antibodies have also been associated with a range of clinical conditions including fetal loss, endocarditis, stroke, heart attack, and hemolytic anemia.
(APS) It is a standard practice in most clinical laboratories to measure and report: both IgG and IgM antiphospholipid antibody levels.
(APS) Anticardiolipin antibodies (aCL) are a heterogeneous group of antibodies (IgG, IgM, and IgA classes). that react with negatively charged phospholipids. autoantibodies directed against cardiolipin is frequently found in systemic lupus erythematosus (SLE) patients.
(APS) • "antiphospholipid antibody syndrome" (APAS).
Thyroglobulin Antibodyare directed against the glycoprotein thyroglobulin located in the thyroid follicles
Levels of thyroglobulin antibodies in serum can also be useful in the assessment of a number of thyroid disorders. 90 percent of patients withMore than autoimmune thyroiditis (Hashimoto's thyroiditis) have thyroglobulin or thyroid microsomal antibodies. While not diagnostic, the detection of thyroglobulin antibodies can aid: 1) in predicting progression of clinical thyroiditis, 2) in further substantiating thyroid disease in patients with non-thyroidal illness, and 3) in predicting postpartum thyroiditis.
Thyroid Peroxidase (TPO) Antibody • The thyroid microsomal antigen has been shown to be the enzyme thyroid peroxidase (TPO). • TPO is a membrane-bound, glycosylated, hemoprotein enzyme , plays a significant role in the biosynthesis of thyroid hormones. • Autoantibodies produced against TPO are capable of inhibiting the enzyme activity. • They are also complement fixing antibodies that can induce cytotoxic changes in cells and are, therefore, a potential cause of thyroid dysfunction. This assay detects anti-TPO autoantibodies.
levels of TPO antibodies in serum can be useful in the assessment of a number of thyroid disorders. More than 90 percent of patients with autoimmune thyroiditis (Hashimoto's thyroiditis) have thyroglobulin or TPO antibodies.
Antibodies to TPO have also been found in most patients with idiopathic hypothyroidism (85%) and Graves' disease (50%), and less frequently in patients with other thyroid disorders. Low titers may also be found in 5-10 percent of normal individuals.
More than 90 percent of patients with autoimmune thyroiditis (Hashimoto's thyroiditis) have thyroglobulin or TPO antibodies.
Antimitochondrial AntibodyPrimarily used when there are symptoms of liver or other organ damage, to confirm a medical diagnosis, or help to identify possible causes of tissue damage.The antimitochondrial antibody test is positive in up to 94% of people with biliary cirrhosis. It is positive in less than 1% of normal people..
Titers (blood levels) of more than 1:160 are generally found only in biliary cirrhosis.Antimitochondrial antibodies are helpful in distinguishing biliary (bile system) cirrhosis from liver problems due to obstruction outside of the liver, viral hepatitis, and alcoholic cirrhosis
Autoimmune liver disease panel (Test)DefinitionAn autoimmune liver disease panel is a series of tests performed when autoimmune liver disease is suspected. These tests include anti-smooth muscle (ASA)antibodies, anti-mitochondrial antibodies(AMA),anti-nuclear antibodies(ANA).
ANTIPARIETAL CELL ANTIBODIESA serologic blood test which measures the presence of antibodies to gastric parietal cells. Less than 2% of the general population will be antibody positive (in the elderly this can be higher).
Stomach mucosa produces a substance called intrinsic factor which is necessary for Vitamin B12 absorption.
Parietal cells secrete • hydrochloric acid • intrinsic factor
Approximately 90% of individuals with pernicious anemia will be antibody positive. A positive result may also be seen in atrophic gastritis, gastric ulcer, thyroid disease, iron deficiency anemia, and diabetes.
Antibodies to parietal cells are present in 80% of adults with pernicious anemia and chronic gastritis; they may participate in the early pathogenesis of parietal cell destruction. They are also present in occasional patients with gastric ulcer or gastric cancer With time, the titer of parietal cell antibodies will decline in some patients with pernicious anemia (possibly related to loss of parietal cells) whereas intrinsic factor antibodies persist.
Glomerular Basement Membrane Antibodies Use Detect the presence of circulating glomerular basement membrane-specific antibodies in Goodpasture syndrome; quantitation may be useful in monitoring treatment. This test is often used in conjunction with the antineutrophil cytoplasmic antibody (ANCA) test for Wegener granulomatosis and vasculitis.