Pediatric Respiratory Physiology
520 likes | 1.64k Views
Pediatric Respiratory Physiology. Drs. Greg and Joy Loy Gordon February 2005. Pediatric Respiratory Physiology. Prenatal – Embryo. Ventral pouch in primitive foregut becomes lung buds projecting into pleuroperitoneal cavity Endodermal part develops into airway alveolar membranes

Pediatric Respiratory Physiology
E N D
Presentation Transcript
Pediatric Respiratory Physiology Drs. Greg and Joy Loy Gordon February 2005
Pediatric Respiratory Physiology Prenatal – Embryo Ventral pouch in primitive foregut becomes lung buds projecting into pleuroperitoneal cavity Endodermal part develops into airway alveolar membranes glands Mesenchymal elements develop into smooth muscle cartilage connective tissue vessels
Pediatric Respiratory Physiology Prenatal Development Pseudoglandular period – starting 17th week of gestation Branching of airways down to terminal bronchioles Canalicular period Branching in to future respiratory bronchioles Increased secretary gland and capillary formation Terminal sac (alveolar) period 24th week of gestation Clusters of terminal air sacs with flattened epithelia
Pediatric Respiratory Physiology Surfactant Produced by type II pneumocytes appear 24-26 weeks (as early as 20 weeks) Maternal glucocorticoid treatment 24-48 hours before delivery accelerates lung maturation and surfactant production Premature birth – immature lungs -> IRDS (HMD) due to insufficient surfactant production
Pediatric Respiratory Physiology Prenatal Development Proliferation of capillaries around saccules sufficient for gas exchange 26-28th week (as early as 24th week) Formation of alveoli 32-36 weeks saccules still predominate at birth
Pediatric Respiratory Physiology Prenatal Development Lung Fluid expands airways -> helps stimulate lung growth contributes ⅓ of total amniotic fluid prenatal ligation of trachea in congenital diaphragmatic hernia results in accelerated growth of otherwise hypoplastic lung (J Pediatr Surg 28:1411, 1993)
Pediatric Respiratory Physiology Perinatal adaptation First breath(s) up to 40 (to 80 cmH2O needed to overcome high surface forces to introduce air into liquid-filled lungs adequate surfactant essential for smooth transition Elevated PaO2 Markedly increased pulmonary blood flow -> increased left atrial pressure with closure of foramen ovale
Pediatric Respiratory Physiology Postnatal development Lung development continues for 10 years most rapidly during first year At birth: 20-50x107 terminal air sacs (mostly saccules) only one tenth of adult number Development of alveoli from saccules essentially complete by 18 months of age
Pediatric Respiratory Physiology Infant lung volume disproportionately small in relation to body size VO2/kg = 2 x adult value => ventilatory requirement per unit lung volume is increased less reserve more rapid drop in SpO2 with hypoventilation
Pediatric Respiratory Physiology Neonate Lung compliance high elastic fiber development occurs postnatally static elastic recoil pressure is low Chest wall compliance is high cartilaginous ribs limited thoracic muscle mass More prone to atalectasis and respiratory insufficiency especially under general anesthesia Infancy and childhood static recoil pressure steadily increases compliance, normalized for size, decreases
Pediatric Respiratory Physiology Infant and toddler more prone to severe obstruction of upper and lower airways absolute airway diameter much smaller that adult relatively mild inflammation, edema, secretions lead to greater degrees of obstruction
Pediatric Respiratory Physiology Control of breathing – prenatal development fetal breathing during REM sleep depressed by hypoxia (severe hypoxia -> gasping) may enhance lung growth and development
Pediatric Respiratory Physiology Control of breathing – perinatal adaptation Neonatal breathing is a continuation of fetal breathing Clamping umbilical cord is important stimulus to rhythmic breathing Relative hyperoxia of air augments and maintains rhythmicity Independent of PaCO2; unaffected by carotid denervation Hypoxia depresses or abolishes coninuous breathing
Pediatric Respiratory Physiology Control of breathing – infants Ventilatory response to hypoxemia first weeks (neonates) transient increase -> sustained decrease (cold abolishes the transient increase in 32-37 week premaures by 3 weeks sustained increase Ventilatory response to CO2 slope of CO2-response curve decreases in prematures increases with postnatal age neonates: hypoxia shifts CO2-response curve and decreases slope (opposite to adult response)
Pediatric Respiratory Physiology Periodic breathing apneic spells < 10 seconds without cyanosis or bradycardia (mostly during quiet sleep) 80% of term neonates 100% of preterms 30% of infants 10-12 months of age may be abolished by adding 3% CO2 to inspired gas
Pediatric Respiratory Physiology Central apnea apnea > 15 seconds or briefer but associated with bradycardia (HR<100) cyanosis or pallor rare in full term majority of prematures
Pediatric Respiratory Physiology Postop apnea in preterms Preterms < 44 weeks postconceptional age (PCA): risk of apnea = 20-40% most within 12 hours postop(Liu, 1983) Postop apnea reported in reported in prematures as old as 56 weeks PCA (Kurth, 1987) Associated factors extent of surgery anesthesia technique anemia postop hypoxia (Wellborn, 1991) 44-60 weeks PCA: risk of postop apnea < 5% (Cote, 1995) Except: Hct < 30: risk remains HIGH independent of PCA Role for caffeine (10 mg/kg IV) in prevention of postop apnea in prematures? (Wellborn, 1988)
Pediatric Respiratory Physiology – Pulmonary and Thoracic Receptors Upper airway Pharyngeal receptors -> inhibition of breathing closure of larynx contraction of pharyngeal swallowing muscles
Pediatric Respiratory Physiology – Pulmonary and Thoracic Receptors Upper airway - Larynx three receptor types pressure drive (irritant) flow (or cold) response to stimulus apnea coughing closure of glottis laryngospasm changes in ventilatory pattern newborn increased sensitivity to superior laryngeal nerve stimulus -> ventilatory depression or apnea H2O more potent stimulus than normal saline ([Cl-])
Pediatric Respiratory Physiology – Pulmonary and Thoracic Receptors Infant (especially preterm) reflex response to fluid at entrance to larynx Normal protective swallowing central apnea (H2O > NS) sneezing laryngeal closure coughing or awakening (less frequent) During inhalation induction pharyngeal swallowing reflex abolished laryngeal reflex intact -> breath holding or central apnea positive pressure ventilation may -> push secretions into larynx -> laryngospasm
Pediatric Respiratory Physiology – Pulmonary and Thoracic Receptors Laryngospasm Sustained tight closure of vocal cords by contraction of adductor (cricothyroid) muscles persisting after removal of initial stimulus More likely (decreased threshold) with light anesthesia hyperventilation with hypocapnia Less likely (increased threshold) with hypoventilation with hypercapnia positive intrathoracic pressure deep anesthesia maybe positive upper airway pressure Hypoxia (paO2 < 50) increases threshold (fail-safe mechanism?) So: suction before extubation while patient relatively deep and inflate lungs and maybe a bit of PEEP at time of extubation
Pediatric Respiratory Physiology – Pulmonary and Thoracic Receptors Slowly adapting (pulmonary stretch) receptors (SARs) Posterior wall of trachea and major bronchi Stimulus distension of airway during inspiration hypocapnia Response inhibit inspiratory activity (Hering-Breuer inflation reflex) May be related to adult apnea with ETT cuff inflated during emergence from anesthesia and rhythmic breathing promptly on cuff deflation
Pediatric Respiratory Physiology – Pulmonary and Thoracic Receptors Rapidly adapting (irritant) receptors (RARs) Especially carina and large bronchi Stimulus lung distortion smoke inhaled anesthetics histamine Response coughing bronchospasm tracheal mucus secretion Likely mediate the paradoxical reflex of Head: with vagal afferents partially blocked by cold, inflation of lungs -> sustained contraction of diaphragm with prolonged inflation may be related to sigh mechanism (triggered by collapse of parts of lung during quiet breathing and increasing surface force) neonatal response to mechanical lung inflation with deep gasping breath
Pediatric Respiratory Physiology – Pulmonary and Thoracic Receptors C-fiber endings (J-receptors) Juxta-pulmonary receptors Stimulus pulmonary congestion edema micro-emboli inhaled anesthetic agents Response apnea followed by rapid, shallow breathing bronchospasm hypersecretion hypotension bradycardia maybe laryngospasm
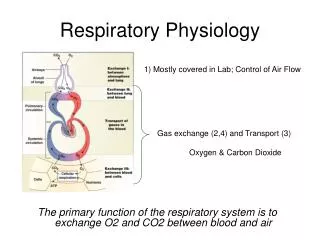
Pediatric Respiratory Physiology – Chemical Control of Breathing Central Chemoreceptors Near surface of ventrolateral medulla Stimulus [H+] (pH of CSF and interstitial fluid; readily altered by changes in paCO2) Response increased ventilation, hyperventilation
Pediatric Respiratory Physiology – Chemical Control of Breathing Peripheral Chemoreceptors Carotid bodies 3 types of neural components type I (glomus) cells type II (sheath) cells sensory nerve fiber endings carotid nerve -> C.N. IX, glossopharyngeal nerve Stimulus paCO2 and pH paO2(especially < 60 mmHg) Response – increased ventilation Contribute 15% of resting ventilatory drive Neonate: hypoxia depresses ventilation by direct suppression of medullary centers
Pediatric Respiratory Physiology – Chemical Control of Breathing
Pediatric Respiratory Physiology – Chemical Control of Breathing Chronic hypoxemia (for years) Carotid bodies lose hypoxemic response E.g., cyanotic congenital heart disease (but hypoxic response does return after correction and restoration of normoxia)
Pediatric Respiratory Physiology – Chemical Control of Breathing Chronic respiratory insufficiency with hypercarbia Hypoxemic stimulus of carotid chemoreceptors becomes primary stimulus of respiratory centers Administration of oxygen may -> hypoventilation with markedly elevated paCO2
Pediatric Respiratory Physiology – Assessment of Respiratory Control CO2 response curve
Pediatric Respiratory Physiology – Assessment of Respiratory Control Effects of anesthesia on respiratory control Shift CO2response curve to right Depress genioglossus, geniohyoid, other phayrngeal dilator muscles -> upper airway obstruction (infants > adults) work of breathing decreased with jaw lift CPAP 5 cmH2O oropharyngeal airway LMA Active expiration (halothane)
Pediatric Respiratory Physiology – Lung Volumes and Mechanics of Breathing = 60 ml/kg infant after 18 months increases to adult 90 ml/kg by age 5 = 50% of TLC may be only 15% of TLC in young infants under GA plus muscle relaxants = 25% TLC
Pediatric Respiratory Physiology – Lung Volumes and Mechanics of Breathing Elastic properties, compliance and FRC Neonate chest wall compliance, CW = 3-6 x CL, lung compliance tending to decrease FRC, functional residual capacity By 9-12 months CW = CL Dynamic FRC in awake, spontaneously ventilating infants is maintained near values seen in older children and adults because of 1. continued diaphragmatic activity in early expiratory phase 2. intrinsic PEEP (relative tachypnea with start of inspiration before end of preceding expiration) 3. *sustained tonic activity of inspiratory muscles (probably most important) By 1 year of age, relaxed end-expiratory volume predominates
Pediatric Respiratory Physiology – Lung Volumes and Mechanics of Breathing Under general anesthesia, FRC declines by 10-25% in healthy adults with or without muscle relaxants and 35-45% in 6 to 18 year-olds In young infants under general anesthesia especially with muscle relaxants FRC may = only 0.1 - 0.15 TLC FRC may be < closing capacity leading to small airway closure atalectasis V/Q mismatch declining SpO2
Pediatric Respiratory Physiology – Lung Volumes and Mechanics of Breathing General anesthesia, FRC and PEEP Mean PEEP to resore FRC to normal infants < 6 months 6 cm H2O children 6-12 cm H2O PEEP important in children < 3 years essential in infants < 9 months under GA + muscle relaxants (increases total compliance by 75%) (Motoyama)
Pediatric Respiratory Physiology – Dynamic Properties Poiseuille’s law for laminar flow: where R resistance l length η viscosity R = 8lη/πr4 For turbulent flow: Rα1/r5 Upper airway resistance adults: nasal passages: 65% of total resistance Infants: nasal resistance 30-50% of total upper airway: ⅔ of total resistance NG tube increases total resistance up to 50%
Pediatric Respiratory Physiology Anesthetic effects on respiratory mechanics Relaxation of respiratory muscles -> decreased FRC cephalad displacement of diaphragm contributes to decreased FRC much less if patient not paralyzed airway closure atalectasis minimized by PEEP 5 cm H2O in children process slowed by 30-40% O2 in N2 (vs 100% O2) V/Q mismatch Endotracheal tube adds the most significant resistance
Pediatric Respiratory Physiology Ventilation and pulmonary circulation Infants: VA per unit of lung volume > adult because of relatively higher metabolic rate, VO2 relatively smaller lung volume Infants and toddlers to age 2 years: VT preferentially distributed to uppermost part of lung
Pediatric Respiratory Physiology Oxygen transport (Bohr effect) = 27, normal adult (19, fetus/newborn)
Pediatric Respiratory Physiology Oxygen transport Bohr effect increasing pH (alkalosis) decreases P50 beware hyperventilation decreases tissue oxygen delivery Hgb F reacts poorly with 2.3-DPG P50 = 19 By age 3 months P50 = 27 (adult level) 9 months P50 peaks at 29-30
Pediatric Respiratory Physiology Oxygen transport If SpO2 = 91 then = PaO2 = Adult 60 6 months 66 6 weeks 55 6 hours 41
Pediatric Respiratory Physiology Oxygen transport P50 Hgb for equivalent tissue oxygen delivery Adult 27 8 10 12 > 3 months 30 6.5 8.2 9.8 < 2 months 24 11.7 14.7 17.6 Implications for blood transfusion older infants may tolerate somewhat lower Hgb levels at which neonates ought certainly be transfused
Pediatric Respiratory Physiology Surfactant Essential phospholipid protein complex Regulates surface tension Stabilizing alveolar pressure LaPlace equation P = nT/r where P ressure r adius of small sphere T ension n = 2 for alveolus Surface tension: 65% of elastic recoil pressure
Pediatric Respiratory Physiology Surfactant Produced by cuboidal type II alveolar pneumocytes (27th week) Lecithin (phosphatidylcholine, PC)/sphingomyelin (L/S) ratio in amniotic fluid correlates with lung maturity
Pediatric Respiratory Physiology Surfactant Synthesis increased by glucocorticoids thyroxine heroin cyclic adenosine monophosphate (cAMP) epidermal growth factor tumor necrosis factor alpha transforming growth factor beta Synthetic surfactant used in treatment of premature infants with surfactant deficiency PPHN CDH meconium aspiration syndrome ARDS (adults and children)
Pediatric Respiratory Physiology – Selected Points Basic postnatal adaptation lasts until 44 weeks postconception, especially in terms of respiratory control Postanesthetic apnea is likely in prematures, especially anemic Formation of alveoli essentially complete by 18 months Lung elastic and collagen fiber development continues through age 10 years Young infant chest wall is very compliant and incapable of sustaining FRC against lung elastic recoil when under general anesthesia, especially with muscle relaxants leading to airway closure and ‘progressive atalectasis of anesthesia’ Mild – moderate PEEP (5 cmH2O) alleviates Hemoglobin oxygen affinity changes dramatically first months of life Hgb F – low P50 (19) P50 increases, peaks in later infancy (30) implications for blood transfusion