Ischemia bowel
Ischemia bowel . Ischemia bowel . "Occlusion of the mesenteric vessels is apt to be regarded as one of those conditions of which the diagnosis is impossible, the prognosis hopeless, and the treatment almost useless " (Cokkinis, 1926). . Ischemia bowel .

Ischemia bowel
E N D
Presentation Transcript
Ischemia bowel • "Occlusion of the mesenteric vessels is apt to be regarded as one of those conditions of which the diagnosis is impossible, the prognosis hopeless, and the treatment almost useless" (Cokkinis, 1926).
Ischemia bowel • inadequate blood flowto or from the involved mesenteric vessels supplying a particular segment of bowel. • The organs typically affected are the small bowel or colon.
Ischemia bowel • Patients with inflammatory bowel disease and infectious colitis can present with similar s/s: cramping abdominal pain, diarrhea, leukocytosis, and hematochezia. Bowel-wall thickening. • however, the pattern of vascular distribution can sometimes narrow the differential diagnosis.
Ischemia bowel • acute or chronic. • arterial or venous • occlusive or nonocclusive.
Pathophysiology • Arterial sources v.s. venous sources: proximately 9:1. Similarly, arterial occlusive disease occurs more frequently than nonocclusive disease approximately 9:1 • The SMA and IMA, and their branches, are more frequently than the celiac artery.
Pathophysiology (a. source) Acute: 1.atheromatous plaque with intimal calcifications 2.embolic from cardiac disease 3. abdominal aortic aneurysms with dissection into SMA 4. hypoperfusion secondary to hypovolemic shock or low-flow cardiac failure.
Pathophysiology (a. source) Chronic : 1.atherosclerosis 2.fibromuscular dysplasia 3.vasculitis. Both occlusive and nonocclusive subtypes can occur .
Pathophysiology (v. source) • are less frequently. • In these cases, bowel ischemia results fromdecreased mesenteric outflow of deoxygenated bloodrather than from decreased perfusion of oxygen-rich blood • Mortality rates generally are low. • SMV is involved more often than the IMV.
Pathophysiology (v. source) • The particular cause often is not clear. • Predisposing risk factors : 1. thrombosis 2. recent abdominal surgery 3. infection 4. hypercoagulable states.
Pathophysiology • Additional rare causes of mesenteric ischemia include : 1.bowel herniation 2. adhesions 3. intussusception 4. antiphospholipid antibody syndrome (APS). APS is associated with hypercoagulable states secondary to circulating immunoglobulins that interact with phospholipids in cell membranes. In a recent study by Kaushik et al, 13 (31%) of 42 patients with APS had CT findings of bowel ischemia.
Acute Ischemia bowel is divided into: 1.Embolic acute mesenteric ischemia 2.thrombolic acute mesenteric ischemia 3. NOMI 4. mesenteric venous thrombosis all types of AMI share many similarities and a final common pathway ( bowel infarction and death, if not properly treated),they are discussed together
1.Embolic acute mesenteric ischemia • has the most abrupt and painful presentation of all types. • abdominal apoplexy. • initial :soft , no tenderness,自覺劇痛程度與理學檢查不成比例 • vomiting and diarrhea (gut emptying) are observed. • most emboli are of cardiac origin ( atrial fibrillation or a recent MI . a history of valvular heart disease or previous embolic episode.)
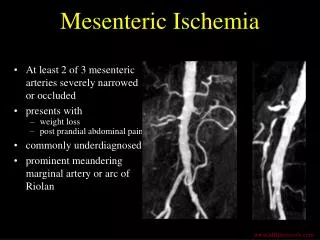
2.Thrombotic acute mesenteric ischemia (TAMI) • happens when an artery already partially blocked by atherosclerosis becomes completely occluded. • 20-50% of these patients have a history of abdominal angina.( postprandial abdominal pain starting soon after eating and lasting for up to 3 hours.) • Weight loss, food fear ,early satiety, and altered bowel habits may be present
2.Thrombotic acute mesenteric ischemia (TAMI) • The precipitating event : 1. a sudden drop in C.O. ( MI or CHF or a ruptured plaque). 2.Dehydration. gradual progression and frequently have a better collateral supply. Bowel viability is better preserved. • Symptoms tend to be less intense and of more gradual onset. • have a history of atherosclerotic disease at other sites or a history of aortic reconstruction
3.Nonocclusive mesenteric ischemia • more frequently in older patients than other forms and often already in an ICU setting . • Symptoms typically develop over several days, and may have had a prodrome ofmalaise and vague abdominal discomfort. • When infarction occurs, increased pain associated with vomiting,hypotensive and tachycardic, with loose bloody stool.
4.Mesenteric venous thrombosis in a much younger patient population than other types . • acute or subacute abdominal pain involvement of the small intestine rather than the colon. • The symptoms are frequently less dramatic. 27% have symptoms for >30 d. • Many patients have a history of the risk factors for hypercoagulability. include oral contraceptive use, deep vein thrombosis (DVT), liver disease, tumor, or portocaval surgery.
Pathophysiology • Large or smaller segments : depending on the location of the occlusion. • mucosal layer becomes anoxic, cell fragility and irreversible cell death. Then, the patient experiences malabsorption, which causes diarrhea and rectal bleeding
Mortality/Morbidity • The major cause of mortality is bowel necrosis • Mortality from all causes is as high as 70%. However, several factors (particularly, the adequacy of collateral vessels) account for variability in mortality rates.
Ischemia bowel • Race: No race predilection is known. • Sex: No sex predilection is known. • Age: Most patients are older than 50 years. Venous causes tend to affect a wider range of patients.
Clinical Details (acute) • Symptoms are usually nonspecific ( D / D with diverticulitis, appendicitis, Crohn disease, peptic ulcer disease, or pelvic inflammatory disease. ) • typical : presents with acute abdominal pain ( initially is characterized as cramping pain, followed by a continuous dull pain. )
Clinical Details (acute) • depending on the particular segment involved, the pain may be morelocalized to one side of the abdomen. • SMA : tends to be more diffuse • IMA: Ischemic pain toward the left side
Clinical Details(acute) • As ischemia progresses, bloody diarrhea, gross bleeding per rectum, and/or leukocytosis are delayed manifestations
Clinical Details (chronic) • postprandial abdominal pain, typically within several minutes of a meal. • reluctant to eat, similar to patients with peptic ulcer disease. • weight loss and chronic diarrhea from malabsorption.
Preferred Examination • history and a physical examination , particularly : 1. the timing of the event. 2.localizing signs and symptoms 3.vascular distribution of the pain. • Unless the patient is unstable, imaging is the criterion standard for diagnosis.
Preferred Examination • 1. Upright and supine plain abdominal radiographs : should be requested first to evaluate for free air, obstruction, ileus, intussusception, or volvulus. • 2. CT by using oral and, preferably, intravenous contrast : may be needed if the cause is not apparent on plain radiographs.
Mesenteric artery ischemia. Radiograph showing bowel spasm, an early sign of ischemia
Mesenteric artery ischemia. Thumbprinting of the bowel.
Mesenteric artery ischemia. Gas in the colon wall, typical of advanced ischemia.
Preferred Examination • 3.Sonography, barium enema study, and angiography : Typically, if additional imaging are needed, ultrasound or angiography is the next step in the workup. MRA is occasionally used to evaluate the patency of the SMA and IMA. It plays a limited role in the diagnosis.
Differential Appendicitis Trauma Pseudomembranous colitis Adenocarcinoma Diverticulitis Crohn Disease Necrotizing Enterocolitis Pneumatosis Intestinalis Typhlitis Ulcerative Colitis
Treatment: • NPO :prepare for surgery and to reduce oxygen demand on the ischemic bowel • surgery • Interventional radiology: angiographic drug infusions or angioplasty.
Treatment: • . acute occlusive mesenteric ischemia : usually surgical resection of the infarcted bowel segment. • Chronic mesenteric ischemia : not a surgical emergency and may be treated conservatively. • Nonocclusive mesenteric ischemia : usually nonsurgically. Depending on the cause
Complications: • Bowel necrosis (requiring bowel resection) • Septic shock • Death • Patients in whom the diagnosis is missed until infarction occurs have a mortality rate of 90%. Even with good treatment, up to 50-80% of patients die. • Survivors of extensive bowel resection face lifelong disability.
Take home message: • Hx: High risk patient ( Af hx, old age, hypercoagulation state…) • PE: Localized pain • Lab: CBC/DC, BCS+e, ABG,amylase ,lipase… • Image (Angiography:唯一可術前診斷確定的方法) • 腹部穿刺:血樣腹水….可確定有infarction • 高度懷疑者:剖腹探查 • Tx: NPO,antibiotics, fluid +electrolite correction, surgery or intervention.術後給予抗凝血劑.